Healing the Gut from the Inside Out: A Functional Medicine Approach to SIBO, IBS, and the Microbiome
Digestive symptoms can quietly take over daily life. Bloating after meals, unpredictable bowel habits, abdominal discomfort, fatigue, and brain fog often linger for years. Many of the patients we see at Vibrant Health of Colorado have already done “everything right.” They have seen specialists, completed scopes and scans, and been told their results look normal, yet they still do not feel well.
A functional medicine approach to gut health looks beyond symptom labels to understand why the gut is struggling in the first place. Our goal is not to silence symptoms temporarily, but to restore balance so the digestive system can function the way it was designed to.
Why Gut Symptoms Persist Even When Tests Look “Normal”
Conventional gastrointestinal testing plays an important role. Colonoscopies, endoscopies, and imaging help rule out serious disease. When those tests come back normal, many people are left with a diagnosis like IBS, or no diagnosis at all, and few next steps.
Irritable Bowel Syndrome (IBS) is a diagnosis of exclusion. It describes a pattern of symptoms, not a single root cause. From a functional medicine perspective, this often means something is not working optimally, even if it is not classified as disease.
In practice, we see many patients whose testing ruled out dangerous conditions, but never explored digestive function, gut motility, microbiome balance, or how stress and hormones are influencing the gut. These gaps are often where answers begin to emerge.
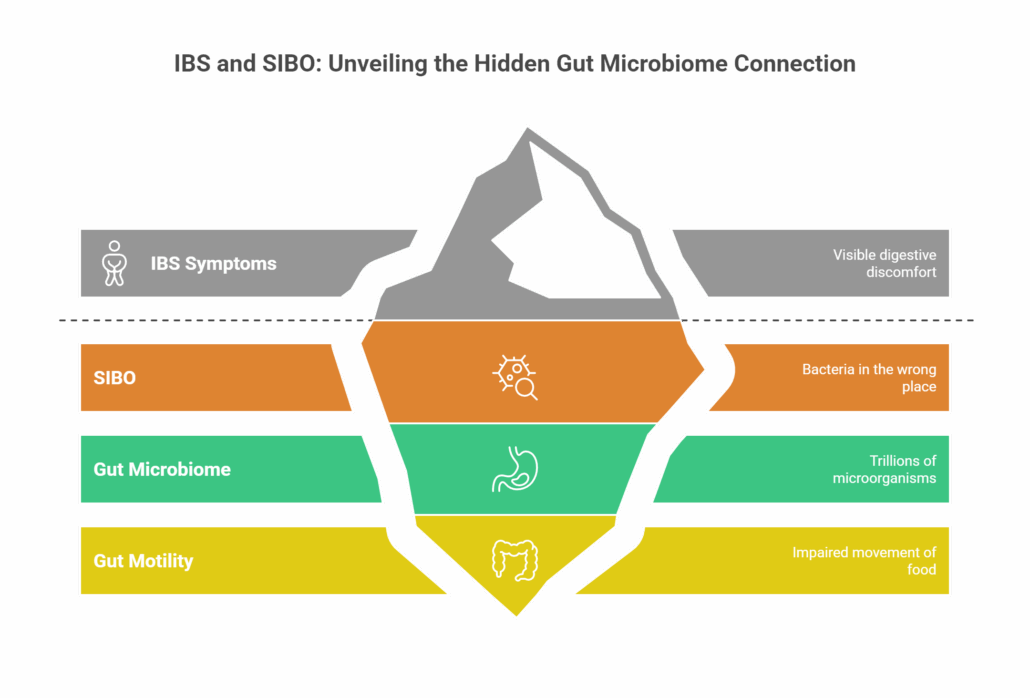
Understanding IBS, SIBO, and the Gut Microbiome
Digestive health terms are often used interchangeably, which can add to confusion. Understanding how these pieces fit together helps create clarity.
IBS, a Symptom-Based Diagnosis
Irritable bowel syndrome is defined by symptoms such as bloating, diarrhea, constipation, abdominal pain, or alternating bowel habits. It does not explain why those symptoms are happening. Many people with IBS have underlying contributors that were never identified.
SIBO, When Bacteria Are in the Wrong Place
Small Intestinal Bacterial Overgrowth (SIBO) occurs when bacteria that belong primarily in the large intestine migrate into the small intestine. This can interfere with digestion and nutrient absorption and commonly causes bloating, gas, abdominal pain, diarrhea, constipation, or both. SIBO frequently overlaps with IBS, and many people carry both labels.
The Gut Microbiome, Your Digestive Ecosystem
The microbiome refers to the trillions of microorganisms living throughout the digestive tract. These microbes influence digestion, immunity, inflammation, metabolism, and even mood. Imbalance, known as dysbiosis, can contribute to chronic gut symptoms and broader health concerns.
These conditions rarely exist in isolation. In real patients, they often overlap and influence one another.

What’s the Link Between SIBO and IBS?
IBS and SIBO are often treated as separate diagnoses, but in functional medicine we frequently see them as closely connected. Many people who carry an IBS diagnosis are later found to have underlying small intestinal bacterial overgrowth contributing to their symptoms.
Rather than viewing this as coincidence, functional medicine recognizes SIBO as a common driver behind many IBS presentations.
Shared Symptoms, Different Labels
IBS is defined by symptoms such as bloating, abdominal pain, gas, diarrhea, constipation, or alternating bowel habits. SIBO can produce those same symptoms when bacteria ferment food in the small intestine, creating excess gas and disrupting normal digestion.
Because the symptoms overlap so closely, SIBO can easily go unrecognized and be labeled as IBS instead.
Why SIBO Is So Common in IBS
In clinical practice and research, a significant portion of people diagnosed with IBS are found to also have SIBO, particularly those with prominent bloating or diarrhea. This helps explain why many IBS treatments focus on symptom management but fail to produce lasting improvement.
When bacterial overgrowth is present, addressing motility, digestion, and microbial balance often leads to meaningful symptom relief.
A Cycle That Feeds Itself
One of the key connections between IBS and SIBO is gut motility.
Impaired motility allows bacteria to remain in the small intestine longer than they should. That overgrowth then produces gas and inflammation, which can further disrupt motility and sensitivity in the gut. Over time, this creates a self-perpetuating cycle of symptoms.
Breaking that cycle often requires more than dietary changes alone.
Why This Connection Matters
When IBS is treated only as a functional diagnosis, care often focuses on managing symptoms rather than identifying what is driving them. Recognizing when SIBO or other forms of microbial imbalance are contributing allows treatment to be more targeted and effective.
For many patients, addressing bacterial overgrowth, supporting motility, and restoring digestive balance can significantly reduce or even resolve symptoms that were previously labeled as IBS.
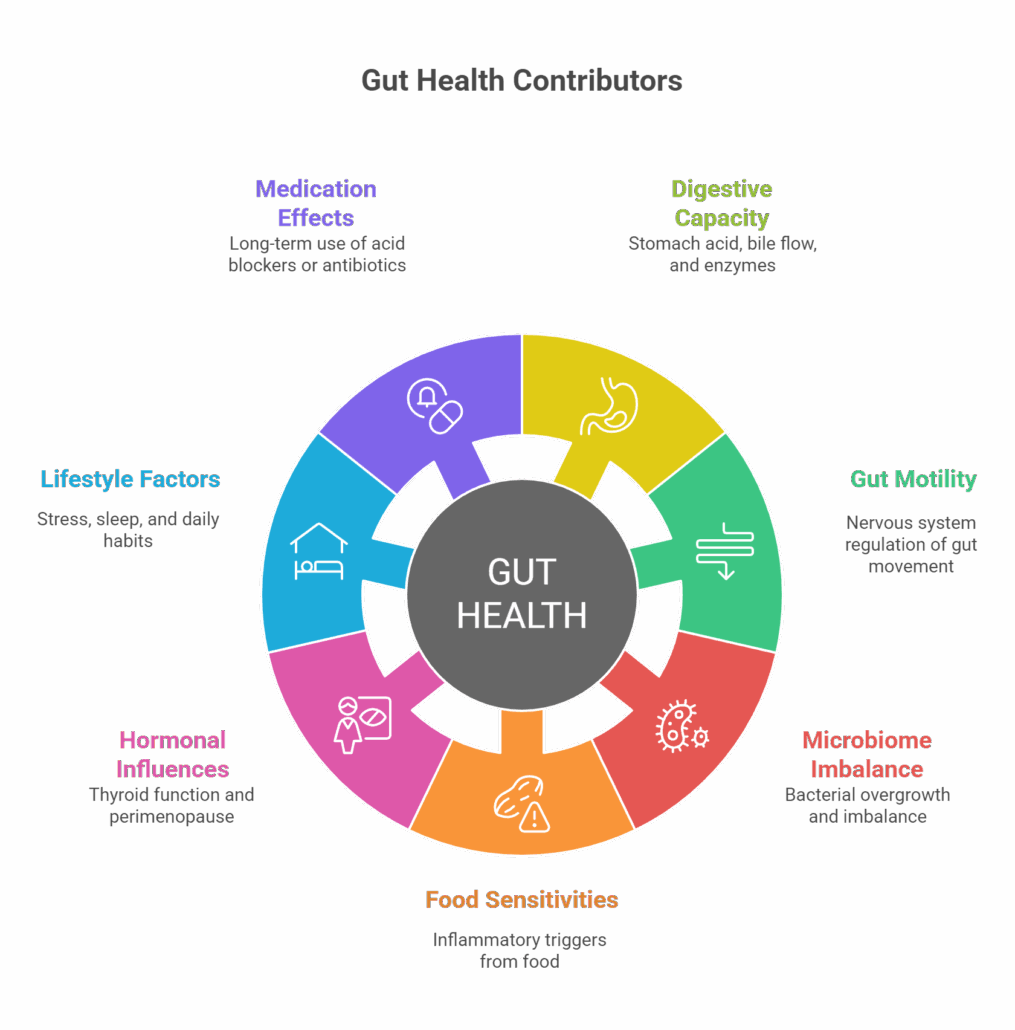
A Functional Medicine View of Root Causes
A functional medicine approach to gut health looks at the gut as part of an interconnected system rather than a standalone organ. Common contributors we evaluate include:
- Digestive capacity, including stomach acid, bile flow, and digestive enzymes
- Gut motility and nervous system regulation
- Microbiome imbalance and bacterial overgrowth
- Food sensitivities and inflammatory triggers
- Hormonal influences, including thyroid function and perimenopause or menopause
- Chronic stress, poor sleep, and lifestyle factors
- Medication effects, such as long-term acid blockers or antibiotics
Rarely is there a single cause. Most people experience a combination of factors that gradually disrupt gut function over time.
How We Evaluate Gut Health at Vibrant Health
We believe comprehensive primary care starts with listening. A thorough history often reveals patterns that testing alone cannot.
When appropriate, we collaborate with gastroenterology to ensure serious conditions are ruled out. From there, we use a selective and intentional approach to functional evaluation. Not every patient needs every test. Testing decisions are based on symptoms, history, and clinical judgment, not checklists.
Equally important is interpretation. Results only matter when they are understood in context and used to guide a personalized plan.
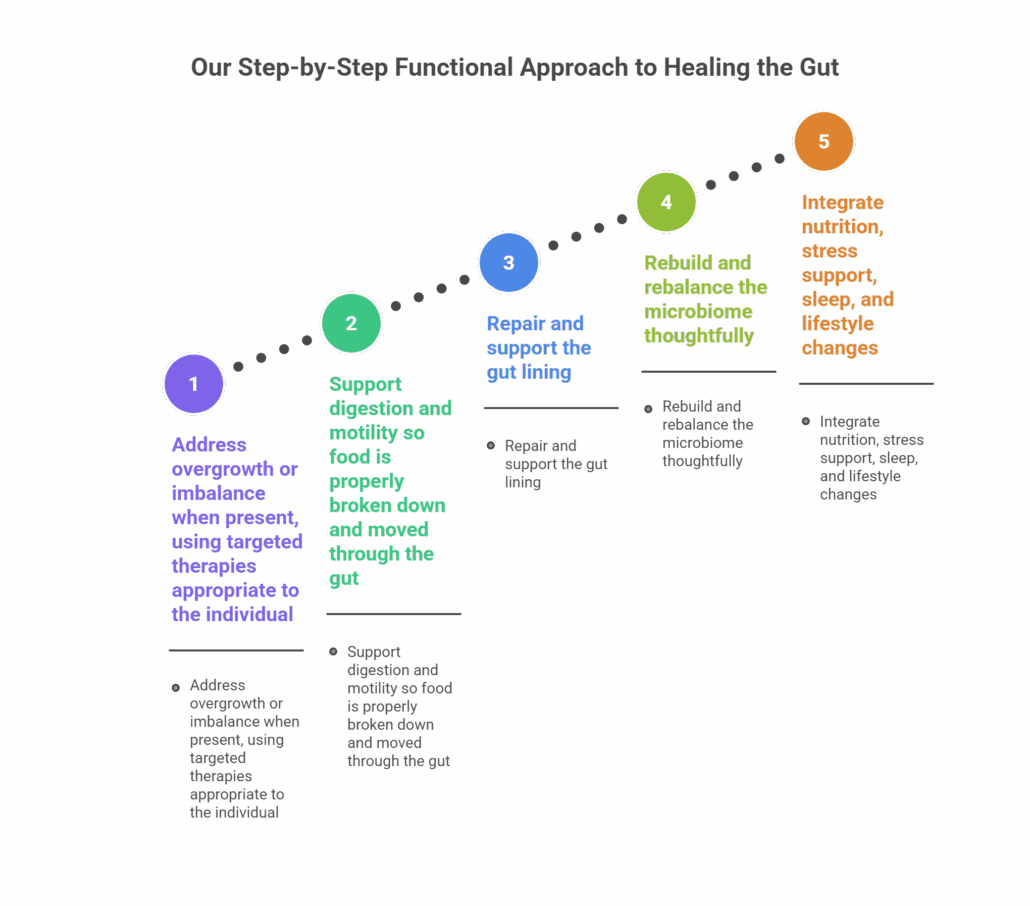
Our Step-by-Step Functional Approach to Healing the Gut
While every plan is individualized, our work generally follows a structured framework:
- Address overgrowth or imbalance when present, using targeted therapies appropriate to the individual
- Support digestion and motility so food is properly broken down and moved through the gut
- Repair and support the gut lining
- Rebuild and rebalance the microbiome thoughtfully
- Integrate nutrition, stress support, sleep, and lifestyle changes
These steps often overlap, and the order may shift based on the person in front of us. Healing is not linear, and adjustments are part of the process.
Tackling IBS and SIBO with a Functional Medicine Framework
IBS and SIBO are often discussed as separate conditions, but in practice they are frequently connected. Many people with IBS symptoms are later found to have bacterial overgrowth, impaired motility, or underlying digestive dysfunction contributing to their symptoms.
With functional medicine, we approach IBS and SIBO through a structured but flexible framework that focuses on restoring normal gut function rather than simply suppressing symptoms. One commonly used model is the 5R framework, which allows us to address the gut systematically while tailoring care to the individual.
Remove
The first step is identifying and reducing factors that are driving irritation or imbalance in the gut. This may include certain fermentable foods, bacterial overgrowth, infections, or other triggers that worsen symptoms such as bloating, pain, or irregular bowel habits.
Dietary strategies are often used short term to reduce symptom burden and bacterial fermentation. These approaches are meant to create relief and insight, not permanent restriction.
Replace
Many people with chronic digestive symptoms are not breaking down food effectively. Low stomach acid, insufficient bile flow, or inadequate digestive enzymes can allow partially digested food to reach the small intestine, where it fuels symptoms.
Supporting digestion appropriately helps the gut do its job more efficiently and reduces stress on the digestive system.
Reinoculate
A healthy gut depends on a diverse and balanced microbiome. Once overgrowth or imbalance is addressed, the focus shifts to supporting beneficial bacteria in a thoughtful way.
This process is highly individualized. Not everyone tolerates probiotics or prebiotics the same way, and timing matters. The goal is balance, not overload.
Repair
Chronic irritation can compromise the gut lining, contributing to inflammation and increased sensitivity. Supporting the integrity of the intestinal lining helps calm the digestive system and improve resilience over time.
This step is especially important for patients who feel reactive to many foods or experience lingering symptoms despite other treatments.
Rebalance
Gut health does not exist in isolation. Stress, sleep quality, movement, and nervous system regulation all play a significant role in digestion and motility.
Addressing these factors is not an optional add-on. It is often essential for preventing recurrence and supporting long-term improvement.
Tools We May Use Along the Way
Depending on symptoms and history, care may include:
- Targeted testing when clinically appropriate, such as breath testing for SIBO
- Short-term, structured dietary strategies guided by clinical context
- Herbal or prescription antimicrobials when overgrowth is identified
- Digestive support to improve breakdown and absorption of food
- Microbiome support introduced carefully and strategically
These tools are never used in isolation. They are combined intentionally and adjusted based on how the body responds.
Nutrition and Gut Healing, Strategy Over Restriction
Diet plays a meaningful role in gut health, but more restriction is not always better.
Short-term therapeutic approaches, such as a low FODMAP diet, or elimination diets, can be useful tools when applied thoughtfully. The goal is symptom relief and insight, not permanent restriction. Long-term avoidance can weaken the microbiome and increase fear around food.
We focus on phased reintroduction, personalization, and sustainability so nutrition supports healing rather than becoming another source of stress.
Preventing Recurrence and Supporting Long-Term Gut Health
One of the most common frustrations we hear is recurrence. Symptoms improve, then slowly return.
Long-term success often depends on addressing factors such as:
- Ongoing gut motility support
- Nervous system regulation and stress resilience
- Hormone balance
- Consistent nutrition and lifestyle foundations
- Follow-up and reassessment as the body changes
Functional medicine is not a one-time fix. It is a partnership focused on long-term stability and resilience.

Is a Functional Medicine Gut Health Approach Right for You
This approach is often helpful for people who:
- Have persistent digestive symptoms without clear answers
- Have tried multiple diets or treatments with limited success
- Want to understand root causes rather than manage symptoms indefinitely
- Are ready for a thoughtful, personalized process
Healing takes time, guidance, and collaboration. Our role is to help you understand what is happening in your body and support you through each step.
Next Steps with Vibrant Health of Colorado
Vibrant Health of Colorado provides functional medicine gut health care alongside comprehensive primary care, gynecology and women’s health services, and hormone optimization.
We see patients along Colorado’s Front Range in Lone Tree, and across the Vail valley in our Eagle location. Additionally, we offer telehealth services across Colorado.
If you are ready to explore a root-cause approach to digestive health and want care that prioritizes listening, clarity, and long-term solutions, contact Vibrant Health of Colorado today.
Frequently Asked Questions About IBS, SIBO, and Functional Medicine
What is the difference between IBS and SIBO?
IBS, or irritable bowel syndrome, is a diagnosis based on symptoms such as bloating, abdominal pain, diarrhea, constipation, or alternating bowel habits. It does not identify a specific cause.
SIBO, or small intestinal bacterial overgrowth, is a condition where bacteria are present in the small intestine in higher-than-normal amounts. This can interfere with digestion and often produces symptoms that look identical to IBS. In functional medicine, SIBO is frequently evaluated as a potential contributor to IBS symptoms rather than viewed as a completely separate issue.
Can treating SIBO improve IBS symptoms?
For many people, yes. When SIBO is contributing to symptoms, addressing bacterial overgrowth, supporting gut motility, and restoring digestive balance can significantly reduce symptoms that were previously labeled as IBS.
However, not all IBS symptoms are caused by SIBO. That is why a personalized evaluation is important rather than assuming a one-size-fits-all approach.
Why do my gut symptoms keep coming back?
Recurrence is common when underlying drivers are not fully addressed. Gut symptoms can return if motility remains impaired, digestion is incomplete, stress remains high, or the microbiome is not adequately supported after treatment.
Long-term improvement often requires addressing these foundational factors alongside any targeted treatment, rather than focusing on short-term symptom relief alone.
Is SIBO the cause of all IBS?
No. While SIBO is common in people with IBS, it is not the cause in every case. IBS can involve multiple overlapping factors, including nervous system regulation, food sensitivities, inflammation, hormonal changes, and prior infections.
Functional medicine focuses on identifying which factors are relevant for each individual rather than assuming the same cause for everyone.
Do I need testing to know if I have SIBO?
Testing can be helpful in some cases, but it is not always required. Breath testing is one tool that may be used when symptoms and history suggest bacterial overgrowth.
At Vibrant Health, testing decisions are made selectively and intentionally. The goal is to gather useful information that guides care, not to order tests automatically.
Is the low FODMAP diet meant to be permanent?
No. The low FODMAP diet is typically used as a short-term therapeutic tool to reduce symptoms and identify triggers. Long-term restriction can negatively affect the microbiome and overall gut health.
A functional medicine approach emphasizes gradual reintroduction and personalization so nutrition remains nourishing, sustainable, and supportive of healing.
How long does it take to heal the gut?
Healing timelines vary depending on the individual, the underlying contributors, and how long symptoms have been present. Some people notice improvement within weeks, while others require a more gradual, step-by-step process over several months.
Functional medicine focuses on steady progress and long-term stability rather than quick fixes.
Can stress really affect my gut that much?
Yes. The gut and nervous system are closely connected. Chronic stress can alter motility, digestion, gut sensitivity, and microbiome balance.
Addressing stress, sleep, and nervous system regulation is often an essential part of improving digestive symptoms, not an optional add-on.
Do probiotics always help with IBS or SIBO?
Not always. While probiotics can be beneficial for some people, others may feel worse if they are introduced too early or in the wrong form.
Functional medicine emphasizes timing, strain selection, and individual tolerance rather than assuming probiotics are appropriate for everyone.
Is functional medicine safe if I have already seen a gastroenterologist?
Yes. Functional medicine is not a replacement for gastroenterology care. It often works alongside conventional evaluation, especially when serious conditions need to be ruled out.
At Vibrant Health, we respect and collaborate with conventional care while addressing functional imbalances that may persist after standard testing is complete.
Who is a good candidate for a functional medicine gut health approach?
This approach is often helpful for people who:
- Have ongoing digestive symptoms despite normal test results
- Have tried multiple diets or treatments without lasting relief
- Want to understand root causes rather than manage symptoms indefinitely
- Are ready to partner in a thoughtful, personalized process

Michelle Sanders is a board-certified Family Nurse Practitioner dedicated to helping patients shift their health trajectory. By bridging the gap between functional and traditional medicine, she specializes in managing chronic conditions, including metabolic disease, cardiovascular health, and thyroid disorders, while emphasizing gut health, hormones, and autoimmune disease. She utilizes a comprehensive range of nutrition, lifestyle changes, and advanced research to help patients reach their goals. A Baylor and Regis University alumna, Michelle practiced internal medicine through a functional lens in Aurora, Colorado prior to joining Vibrant Health. When not with her husband and three children, she enjoys hiking, playing pickleball, tending to her “plant babies,” and staying active in her church.




