Autoimmune Thyroid Disease Explained: How Functional Medicine Treats Hashimoto’s and Hypothyroidism at the Source
Autoimmune thyroid disease is one of the most common yet misunderstood chronic conditions we see in practice. Many patients are told they have hypothyroidism. Others are diagnosed with Hashimoto’s thyroiditis. Some are simply told their labs are “normal,” even though they feel exhausted, foggy, anxious, or unlike themselves.
If this sounds familiar, you are not alone.
At Vibrant Health of Colorado, we believe thyroid disease deserves a deeper explanation. When patients understand what is happening inside their bodies, they are better equipped to move forward with clarity and confidence.
This article explains what autoimmune thyroid disease truly is, how Hashimoto’s and hypothyroidism develop, why conventional treatment often leaves patients symptomatic, and how a functional medicine approach addresses the root contributors driving thyroid dysfunction.

What Is Autoimmune Thyroid Disease?
The thyroid is a small butterfly-shaped gland located at the base of the neck. It produces hormones that regulate metabolism, temperature control, brain function, cardiovascular health, digestive motility, menstrual cycles, and energy production.
The two primary thyroid hormones are:
- T4, also called thyroxine
- T3, the active hormone that influences cells throughout the body
Hypothyroidism occurs when the thyroid gland does not produce enough hormone to meet the body’s needs. When thyroid hormone levels decline, metabolism slows. This can lead to symptoms such as:
- Persistent fatigue
- Weight gain or difficulty losing weight
- Brain fog
- Depression or low mood
- Hair thinning
- Constipation
- Cold sensitivity
- Irregular or heavy menstrual cycles
- Reduced exercise tolerance
However, not all hypothyroidism has the same cause.
Hashimoto’s thyroiditis is an autoimmune condition. In Hashimoto’s, the immune system mistakenly identifies thyroid tissue as foreign and begins attacking it. Over time, this immune assault damages the gland and reduces its ability to produce hormones. Hashimoto’s is the most common cause of hypothyroidism in the United States.
This distinction is essential; Hypothyroidism describes low thyroid function, while Hashimoto’s describes the immune process causing that dysfunction.
Treating hypothyroidism without addressing Hashimoto’s is like refilling a leaking tank without repairing the leak.
How Hashimoto’s and Hypothyroidism Develop
Autoimmune thyroid disease typically develops through a combination of genetics and environmental influences. Most individuals who develop Hashimoto’s have a genetic predisposition, but genes alone do not determine destiny.
Three broad elements often interact:
- Genetic susceptibility
- Environmental or physiological triggers
- Immune dysregulation
Over time, immune imbalance may lead to the production of thyroid antibodies, most commonly thyroid peroxidase antibodies and thyroglobulin antibodies. These antibodies signal that the immune system is targeting thyroid tissue.
In early stages, thyroid hormone levels may still fall within laboratory reference ranges. Patients may experience symptoms long before TSH becomes abnormal. Eventually, as thyroid tissue is damaged, hormone production declines and hypothyroidism becomes measurable.
This progression helps explain why some patients feel unwell for years before receiving a formal diagnosis. It also explains why focusing only on TSH can miss early autoimmune activity.
Understanding Hypothyroidism Beyond a Lab Number
TSH, or thyroid stimulating hormone, is commonly used to assess thyroid function. When thyroid hormone levels decline, TSH rises in an effort to stimulate the gland.
While TSH is useful, it is only one piece of the picture.
Comprehensive thyroid assessment may include:
- TSH
- Free T4
- Free T3
- Thyroid antibodies
Some individuals convert T4 into T3 less efficiently. Others may have hormone levels within range but still experience symptoms due to inflammation, nutrient deficiencies, or metabolic dysfunction.
Hypothyroidism is not just a number. It is a clinical condition influenced by immune health, stress physiology, gut integrity, nutrient availability, and hormonal balance.
Why Traditional Medical Management Often Falls Short
Conventional treatment for hypothyroidism typically involves prescribing synthetic T4 hormone, most commonly levothyroxine. This approach is appropriate and necessary in many cases. Severe hypothyroidism can have significant health consequences if untreated.
However, traditional management often stops at hormone replacement.
Common limitations include:
- Antibodies may not be regularly monitored.
- Nutrient status is rarely assessed.
- Gut health is not evaluated.
- Inflammation drivers are not explored.
- Stress physiology is overlooked.
- Lifestyle contributors are not addressed.
When TSH falls within the reference range, treatment is often considered complete, Yet many patients continue to experience fatigue, mood instability, cognitive fog, and weight resistance despite normalized labs.
Medication restores hormone levels. It does not regulate the immune system. Nor does it reduce chronic inflammation or repair intestinal permeability. This gap is where functional medicine provides depth.
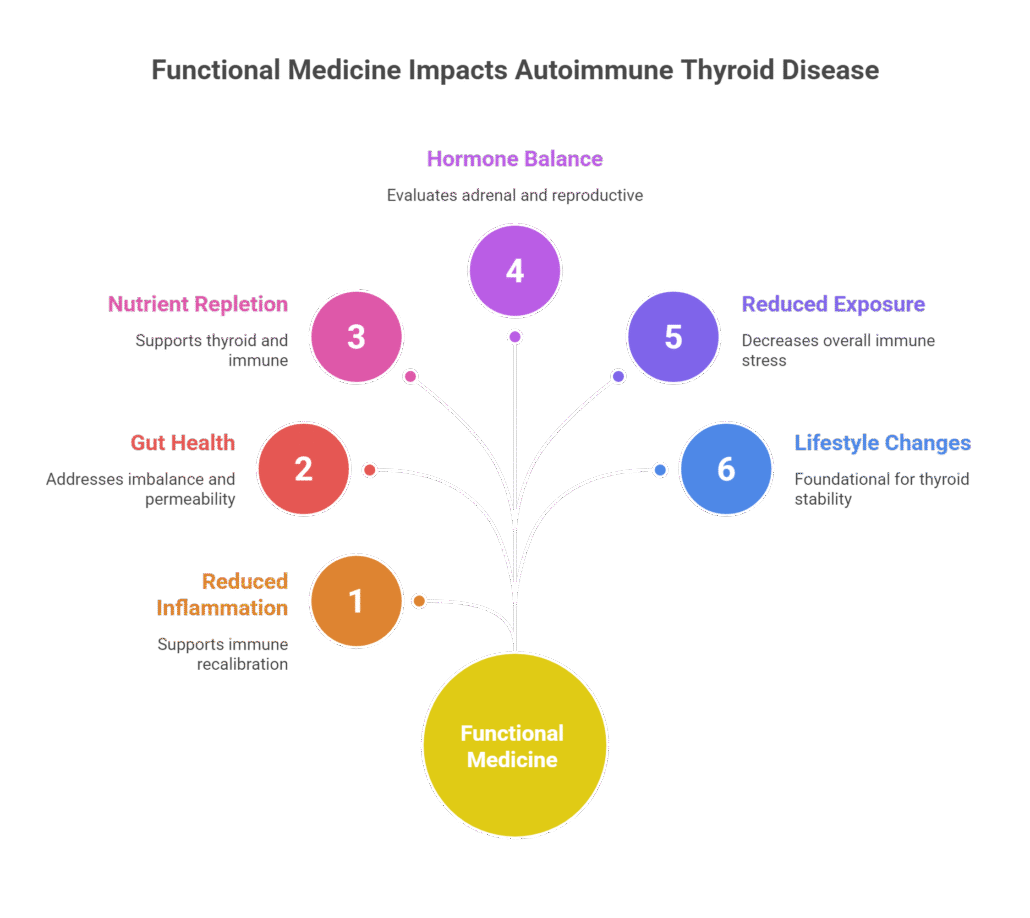
A Functional Medicine Framework for Autoimmune Thyroid Disease
Functional medicine views Hashimoto’s and hypothyroidism as systemic conditions rather than isolated gland disorders. The thyroid does not operate independently. It responds to immune signals, metabolic demands, hormonal shifts, and environmental inputs.
At Vibrant Health, we approach autoimmune thyroid disease through interconnected systems.
Chronic Inflammation
Autoimmune disease is inherently inflammatory. Inflammation may be influenced by diet quality, blood sugar instability, sleep deprivation, toxin exposure, or chronic stress.
Reducing inflammatory burden supports immune recalibration and protects remaining thyroid function.
Gut Imbalance and Intestinal Permeability
The majority of immune activity originates in the gut. When intestinal barrier integrity is compromised, immune activation increases.
A functional approach and evaluation to gut health and the microbiome may include:
- Microbiome analysis
- Markers of gut inflammation
- Digestive function assessment
Addressing gut imbalance often plays a central role in autoimmune hypothyroidism treatment.
Nutrient Deficiencies
Thyroid hormone production and immune regulation depend on adequate levels of:
- Selenium
- Zinc
- Iron
- Vitamin D
- B vitamins
Even subtle deficiencies can impair hormone conversion or exacerbate inflammation.
Personalized nutrient repletion supports both thyroid and immune function.
Hormonal Interactions and Cortisol
Chronic stress elevates cortisol. Persistent cortisol dysregulation can impair T4 to T3 conversion and worsen inflammation.
In women, perimenopause and menopause add complexity. Estrogen fluctuations can influence thyroid hormone binding and symptom patterns.
A whole-person approach to hormone health evaluates adrenal resilience and reproductive hormone balance alongside thyroid function.
Environmental Exposures
Certain environmental chemicals may disrupt endocrine signaling. While complete avoidance is unrealistic, reducing cumulative exposure and supporting detoxification pathways may decrease overall immune stress.
Lifestyle Foundations
Sleep, movement, stress resilience, and nutrient-dense eating patterns shape immune regulation. Sustainable lifestyle changes are foundational in long-term thyroid stability.
Functional Medicine Testing Tools
A root-cause approach begins with a thorough evaluation.
Testing may include:
- Full thyroid panel with antibodies
- Iron studies
- Vitamin D levels
- Inflammatory markers
- Blood sugar and metabolic markers
- Cortisol patterns when indicated
- Comprehensive stool analysis in select cases
Testing is individualized. It is not about excess. It is about relevance and interpretation within the clinical picture.
Understanding patterns allows us to design precise, targeted interventions.
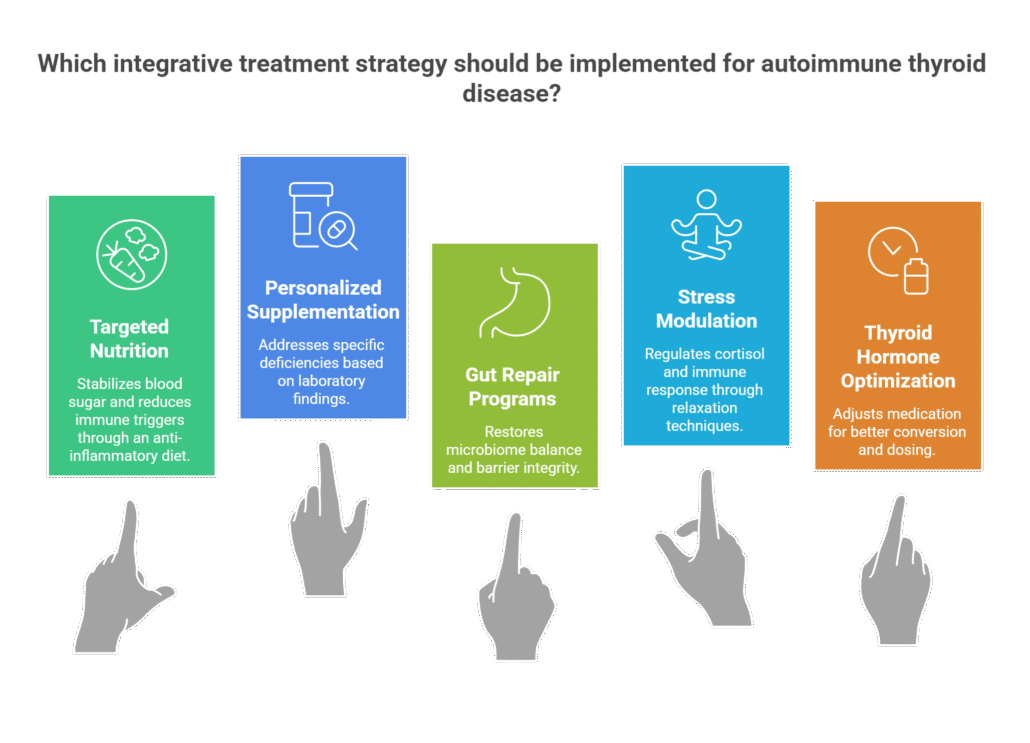
Integrative Treatment Strategies
Treatment plans are customized and phased. Autoimmune conditions require patience and consistency.
Common strategies include:
Targeted Nutrition
- An anti-inflammatory dietary pattern stabilizes blood sugar and reduces immune triggers. In some cases, structured elimination protocols help identify specific sensitivities.
Personalized Supplementation
- Supplements are selected based on laboratory findings and symptom patterns. The goal is strategic repletion, not generic protocols.
Gut Repair Programs
- When intestinal imbalance is identified, phased protocols may support microbiome restoration and barrier integrity.
Stress Modulation
- Breathwork, structured recovery practices, sleep optimization, and mind-body therapies help regulate cortisol and immune response.
Thyroid Hormone Optimization
- Medication adjustments are made carefully when necessary. Some patients benefit from evaluating conversion patterns or refining dosing strategies in collaboration with appropriate medical oversight.
Functional medicine complements, rather than replaces, responsible hormone therapy.
A Realistic Patient Journey
Many patients arrive frustrated. They are taking medication but still feel unwell. After comprehensive evaluation, we often uncover layered contributors such as iron deficiency, elevated antibodies, disrupted sleep, chronic stress patterns, or gut imbalance.
As these factors are addressed gradually, patients commonly report:
- More stable energy
- Improved mental clarity
- Better mood resilience
- Reduced inflammation
- Improved weight regulation
Progress is steady, not instantaneous. Autoimmune disease develops over time and requires thoughtful, long-term support.

Functional Medicine and Conventional Primary Care Can Work Together
It is important to emphasize that functional medicine does not replace necessary medical care.
If thyroid hormone levels are low, replacement therapy is often essential. Severe hypothyroidism requires careful management.
In some cases, endocrinology referral is appropriate, particularly with nodules, complex lab patterns, or unusual presentations.
Functional medicine adds depth. It addresses immune triggers, metabolic stressors, nutrient status, and lifestyle foundations that influence long-term outcomes.
The most effective care is often collaborative and integrative.
Moving Forward With Clarity
Autoimmune thyroid disease affects energy, cognition, mood, metabolism, and quality of life. It can be discouraging to feel symptomatic despite being told your labs are stable.
Understanding the immune basis of Hashimoto’s reframes the condition. Hypothyroidism is not simply a hormone deficiency. It is often the downstream result of immune dysregulation.
At Vibrant Health of Colorado, we combine comprehensive primary care with a systems-based functional medicine approach. We evaluate immune drivers, metabolic health, hormonal balance, nutrient status, and lifestyle factors alongside thyroid hormone levels.
Our goal is not only normalized labs, our goal is restored resilience.
If you are navigating Hashimoto’s or hypothyroidism and are ready for a more comprehensive approach, we are here to partner with you.
We see patients along Colorado’s Front Range in Lone Tree, and across the Vail valley in our Eagle location. Additionally, we offer telehealth services across Colorado.
If you are ready to explore a root-cause approach to digestive health and want care that prioritizes listening, clarity, and long-term solutions, contact Vibrant Health of Colorado today.
Healing takes time, and progress is possible. With the right framework, many patients rediscover energy, clarity, and a renewed sense of vitality.

Deanna Woodroffe, WHNP, is the founder of Vibrant Health of Colorado and a passionate Women’s Health Nurse Practitioner with a focus on functional and integrative medicine. Early in her career, she became frustrated with the inability of traditional medicine to treat her patients’—and her own—chronic symptoms, driving her to pursue a fellowship in Anti-Aging and Functional Medicine. With over twenty years of experience, Deanna helps patients resolve complex, chronic symptoms by focusing on root causes and restoring balance to the body. Her comprehensive approach utilizes bio-identical hormone therapy, thyroid optimization, and addressing lifestyle factors like nutrition and stress to return her patients to feeling vibrant.





Leave a Reply
Want to join the discussion?Feel free to contribute!